When a doctor told 19-year-old Sidney in 2004 that he had cancer, he says time seemed to freeze. Sitting in a hospital room in Nairobi, Kenya, Sidney was blindsided by despair and struggled to process the diagnosis.
He had just finished high school and had earned a scholarship to study aeronautical engineering, with dreams of attending university in the United States. Suddenly, he felt everything was put on pause.
Closing the gaps in cancer care
Every three minutes, a child is diagnosed with cancer worldwide.
Cancer rates in the Commonwealth have soared by 35 percent between 2008 and 2018, with a further 35 percent rise expected by 2030. Concurrently, funding for cancer care is shrinking as Overseas Development Aid is redirected to issues outside the health sphere, leaving families in low- and middle-income countries (LMICs) increasingly on their own.
The gap between those who can access treatment and those who cannot is widening. Despite these daunting statistics, a young Kenyan, Sidney Chahonyo, is working tirelessly to close the gaps in cancer care and support for young people.

As his friends departed for new campuses, Sidney stayed behind with his symptoms: a runny nose, flu-like fatigue, nosebleeds, sharp headaches, and, ultimately, a growing tumour. Before that fateful 2004 diagnosis, he spent months shuttling between clinics, receiving repeated treatments for sinus issues, never realising he was battling something far more sinister.
"Take this pill for 15 days, and you'll be fine," doctors would tell him, handing out medication after medication to reassure him. Six months and countless medications later, an Ear, Nose and Throat specialist finally took his symptoms seriously. Tests followed: blood work, CT scan, MRI and biopsy. The result was cancer of the post-nasal space, where the ear, nose and throat converge.
"I remember feeling utterly lost. I was desperate for any plan, and prayed for an affordable one," Sidney recalls in a recent interview with the Commonwealth Secretariat.
Fortunately, the oncologist to whom he was referred had treated similar cases and, despite the six-month delay, remained optimistic about Sidney’s chances. Treatment began with radiotherapy, followed by monthly cycles of chemotherapy. Beyond the physical agony, panic struck when medication could not be sourced locally. Sidney’s family became his lifeline, searching for drugs across South Africa, Europe, and the United States, finally securing what he needed in Dubai at US $400 a dose. Most families cannot.

The prolonged delays and the difficulty in accessing timely and affordable treatment are a painful reminder of the massive inequality that continues to shape cancer, particularly in LMICs. The six‑month delay is a symptom of a systemic weakness, one that arises when early signs of cancer go unrecognised in health systems with limited specialist capacity, and where patients lack the financial means or influence to secure thorough diagnostic follow‑up.
During his treatment, Sidney saw how families were thrust into poverty with exorbitant cancer diagnoses. In some cases, parents have to choose between medication and food. The cost of care functions as a sentence, not just an obstacle.
“I do not know what would have become of me if my family had not made sacrifices and rallied behind me financially. I am one of the lucky ones – how many young people can be as lucky?”
A journey of resilience, advocacy and hope
Today, Sidney is cancer-free, but not untouched by its shadow. About 18 years after his recovery, the side effects of radiotherapy resurfaced. His hearing dropped dramatically just as he started a new job in 2017. Unable to meet the demands of the role, he lost it. A hearing aid helped him regain his footing, but it sharpened a conviction that had been growing since his diagnosis.
"Surviving cancer isn’t the finish line. What you do with your survival is what matters."
That belief propelled Sidney to Kenyatta National Hospital, Kenya’s largest referral hospital, where he volunteered in the paediatric oncology ward. He supported children and families gripped by the same fear he once faced.

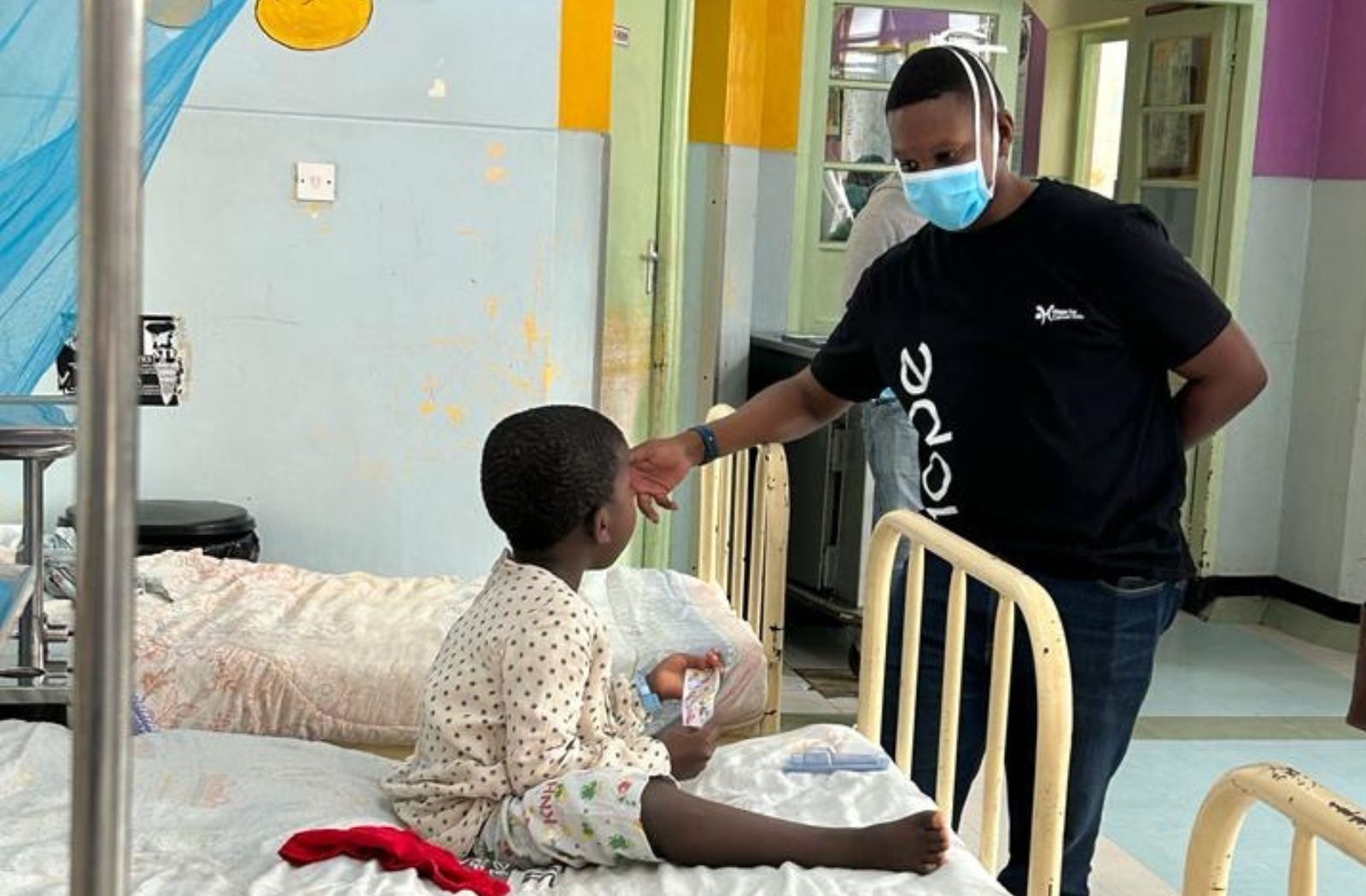
Inspired further, he joined a local charity, Hope for Cancer Kids - a non-profit organisation dedicated to providing support, resources, and hope to families affected by childhood cancer - first as board chair, later as Executive Director, and currently as Fundraising Director. The charity funds national insurance premiums, provides transport and accommodation, and covers other out-of-pocket expenses, including diagnostics, lab work and clinic fees.
Through this charity, Sidney helps ensure that geography and poverty are not the deciding factors in whether a child lives or dies.
"I am inspired by the need to translate words beyond empathy into action: treatment, transport, nutrition support, and hope. I am using my story not just to create awareness, but to push for child-friendly National Cancer policies as countries develop their National Cancer Control Programmes."
The Commonwealth connection
For Sidney, the chance to speak at the 2012 London Global Cancer Week organised in partnership with the Commonwealth Secretariat was pivotal.
"Connecting through the Commonwealth projected my work onto a larger stage. The Secretariat, through avenues like the International Cervical Cancer Task Force, has been a springboard, introducing me to a dynamic community determined to make a difference," he reflects.
That exposure, he adds, unlocked collaborations and funding conversations previously out of reach.

It empowered Sidney to advocate not just for individual children, but for stronger cancer care systems and sustainable support for families. He notes that these partnerships have strengthened the credibility and visibility of his programmes and amplified their impact.
For Sidney, the upcoming Commonwealth Health Coordination Forum presents an important opportunity to bring the realities of young cancer patients in Kenya to the global stage. The forum will allow him to share the voices of young patients, his experience, learn from others, and build new partnerships to support resource mobilisation.
The forum, taking place ahead of the 79th World Health Assembly in May, will bring together Commonwealth senior officials, health ministers, advocates and practitioners. Delegates will share best practices and scalable solutions to strengthen cancer prevention, early detection, treatment and care across diverse Commonwealth contexts amid persistent funding gaps.
They will also hear findings from the Lancet Oncology Commission on Cancer in the Commonwealth, including new evidence and tools to support collaboration on cancer care.
At a time when funding for cancer care in the developing world is shrinking, precisely when it needs to expand, resource gaps continue to translate into delayed diagnoses, limited access to treatment, and preventable loss of life.
Sidney believes that if cancer care is shaped by advocates like him, those who turn personal adversity into collective action, the Commonwealth can move closer - and more quickly - towards delivering affordable care and reducing preventable suffering and deaths.
Find out how we are shaping the future of cancer care across the Commonwealth
2026 Inaugural Commonwealth Health Coordination Forum
Ahead of the 79th World Health Assembly, health ministers and senior officials will convene in Geneva for the first Commonwealth Health Coordination Forum (CHCF) to shape the Commonwealth's cancer agenda.
Read more





